‘The future ain’t what it used to be.’ -Yogi Berra
Dr. Jonathan L. Nicozisis discusses a product that facilitates true tissue remodeling preceding force application
The history chapters of orthodontic textbooks have taught us much on the evolution of our industry. Debates and understanding of growth and development, extraction versus non-extraction, expansion at all costs versus expansion at your own peril, etc., have run their course. Some decide to continue in such debate for the mental exercise or personal benefit as new tools for measurement and imaging continue the ability to kick the can of promising and definitive answers down the proverbial road.
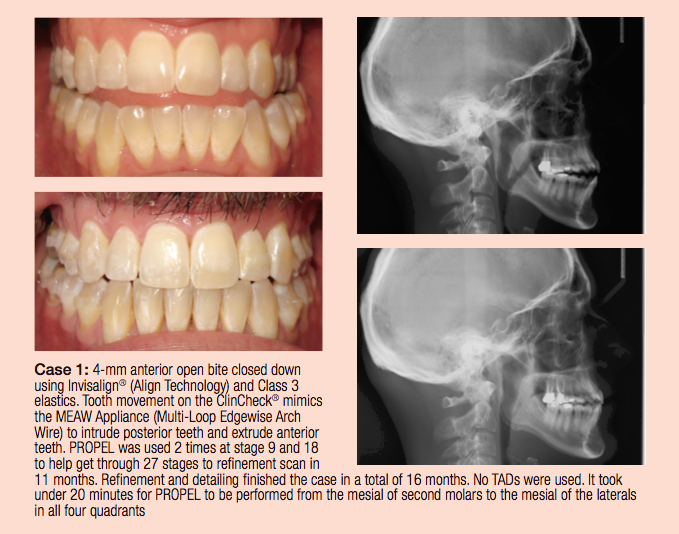 Likewise the merits and advantages of appliance systems over others have provided much pulp for collegiate discourse. Often when talking about tip, torque, and rotational control, we forget the simplicity of the dichotomy of tooth movement; we focus in on bracket design, slot size, slot width, twin wing, single wing, active clip, passive clip, torque in the base, torque in the face, etc., to best control the first, second, and third orders of movements.
Likewise the merits and advantages of appliance systems over others have provided much pulp for collegiate discourse. Often when talking about tip, torque, and rotational control, we forget the simplicity of the dichotomy of tooth movement; we focus in on bracket design, slot size, slot width, twin wing, single wing, active clip, passive clip, torque in the base, torque in the face, etc., to best control the first, second, and third orders of movements.
The future of orthodontics used to be about these arguments.
When one zooms the focus out of these debates, attention is brought back to the biologic system involved with the physiology of tooth movement. We then realize the wide open territory of creating the ability to proactively augment a patient’s biology to facilitate and stabilize tooth movement. This might be considered the “fourth order” of orthodontics: harnessing and augmenting the biology of tooth movement to our advantage. Currently, we talk to teeth and host tissues by applying forces and the periodontium, and teeth react after the fact. When one thinks about it, this is truly an unsophisticated way to talk to teeth. It would be to our advantage and a true paradigm shift in orthodontics to have the host tissues react prior to force application.
Linge (1976) concluded that mechanical properties of the host tissue determine the characteristics and distribution of mechanical forces at the site of tissue reactions. It is the alteration of these tissue mechanical properties with treatment adjuncts that is attractive to the clinician. Having this ability enables the clinician to directly affect tissue response rather than doing it indirectly through secondary forces from the tissue resistance. To that end, tissue response could therefore be changed from a pattern of tissue damage repair following force application to that of true tissue remodeling preceding force application.
What used to be considered science fiction is now a reality.
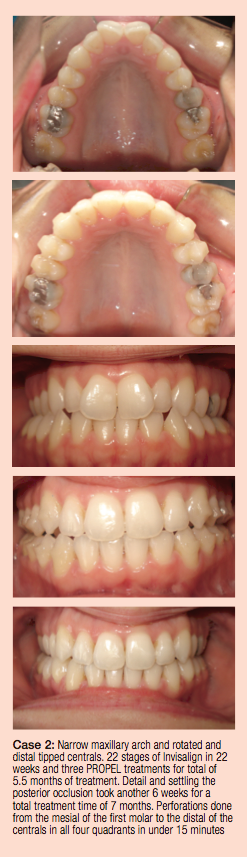 Previous attempts to this end have been tried and documented. “Electric braces” proved to be ineffective, and after a completed human clinical trial, the naturally occurring protein relaxin as a therapeutic adjunct to facilitate and stabilize tooth movement succumbed to the FDA’s stifling wave of resistance.
Previous attempts to this end have been tried and documented. “Electric braces” proved to be ineffective, and after a completed human clinical trial, the naturally occurring protein relaxin as a therapeutic adjunct to facilitate and stabilize tooth movement succumbed to the FDA’s stifling wave of resistance.
Surgical techniques involving full thickness flaps and corticotomies or piezoelectric corticotomies are well-known and effective but carry their own negatives. Patients’ acceptance can be limited due to expense, the invasive nature of the procedure, and length of recovery time and discomfort following the procedure.
Vibration devices delivering pulsatile forces have also been investigated and are now commercially available. The original research behind this technology investigated the application of pulsatile forces’ effects on the sagittal growth of the premaxillae and premaxillary sutures in rabbits. These suture responses, results, and conclusions from this research were then applied to the response of the periodontal ligament involved in tooth movement. While having some similarities in tissue composition, suture growth, and suture response to orthopedic forces (with or without vibration) is very different than that of the periodontal ligament in homeostasis or in response to the influence of orthodontic forces. Nevertheless, the marketplace has a product with an FDA Class 2 medical device designation that is approved to be used with fixed braces.
Fast forward to 2011 when technology developed at NYU’s Department of Orthodontics and licensed by PROPEL Orthodontics allows us to cross the threshold into the fourth order of orthodontics; host tissue remodeling prior to force application to facilitate tooth movement. Without a surgical flap, PROPEL Orthodontics’ proprietary technology, the Excellerator, creates micro-osteoperforations through both fixed and movable mucosa, into the bone between the roots of the teeth. These micro-osteoperforations go through the cortical bone and into the medullary bone. In doing so, the Excellerator stimulates the local inflammatory response and increases expression of cytokines and other secondary messengers at the cellular level. This increase in cytokine expression causes an increase in recruitment and differentiation of osteoclasts which in turn causes an expedited rate of bone remodeling to occur. The end result is faster tooth movement.
Truly, now tissue response can be changed from a pattern of tissue-damage-repair following force application to that of true tissue remodeling preceding force application. This is the new fourth order of orthodontics and PROPEL’s technology delivers it in an effective, efficient, and safe manner.
PROPEL has been widely accepted by both clinicians and patients. Clinicians have accepted the treatment for its characteristics, which include ease of use, the ability to be in full control without relying on patient compliance, and the capability of applying it in a targeted area of the mouth rather than vibrating the whole dentition when that might cause anchorage concerns or excessive mobility. Patients have accepted PROPEL for its reasonable cost, lack of recovery from a surgical procedure, and ability to go about their day’s activities immediately following the office visit.
Research shows that Excelleration should be repeated until the desired tooth movement is accomplished, the frequency of which is about once every 8 to 12 weeks. This translates to using one to three devices for an average case. That means an extra $100-$300 to save half the number of office visits for the case. The Excellerator is the only patented device specifically designed to perform transmucosal osteoperforations. All other protocols would be using that instrumentation in an off-label manner, thus exposing oneself to liability issues.
The November 2013 issue of the American Journal of Orthodontics and Dentofacial Orthopedics (AJODO) has the first published clinical trial study for PROPEL and the impact micro-osteoperforations (MOPs) have on tooth movement. The conclusions from the study show that micro-osteoperforations significantly increased the expression of cytokines and chemokines known to recruit osteoclast precursors and stimulate osteoclast differentiation. They also increased the rate of canine retraction 2.3-fold compared with the control group. Patients reported only mild discomfort locally at the spot of the MOPs with little to no pain experienced at days 14 and 28. It was concluded that micro-osteoperforations are an effective, comfortable, and safe procedure to accelerate tooth movement during orthodontic treatment and could reduce orthodontic treatment time by 62%.
The Excellerator device itself is a Class 1 FDA-registered medical device that is indicated to be used with any orthodontic modality of treatment. Its surgical-grade stainless steel tip will not break during use. Depths of 3 mm, 5 mm, and 7 mm can be selected by the doctor depending on where in the mouth the perforations are to be performed. Once that depth is reached, a red indicator light turns on alerting the clinician that the desired depth has been reached and the device can then be removed by turning it counterclockwise before proceeding to the next perforation site. Finally, the driver tip is encased in a retractable sheath that helps hold the gingival tissue taut preventing excessive tissue stretching and tearing. It is indicated to do two to three perforations per site between each set of roots starting in the fixed tissue and going as apical as reasonably possible. The effect of increased inflammatory response has been measured to radiate 6 mm-10 mm around the perforation site.
Protocol for anesthesia and sepsis control is the same for TAD placement. A profound gel anesthesia or local anesthesia is sufficient along with rinsing with Chlorhexidine for a minute before and after.
Such sophisticated yet simple technology based on a sound foundation of basic science has allowed us to bridge the gap between our basic science research and clinical application of that research. As such, this paradigm shift once thought of as science fiction, is now a reality as Excelleration allows the host tissues to be proactive rather than reactive to the forces we impart on them. The end result is better outcomes and faster treatment incorporating an adjunct to therapy that has been found to be safe, effective, efficient, and reasonably priced ensuring broad acceptance. Yogi Berra was right in saying that the future ain’t what it used to be. The time for the fourth order of orthodontics has come, and PROPEL is carving this path with more developing technology to follow.
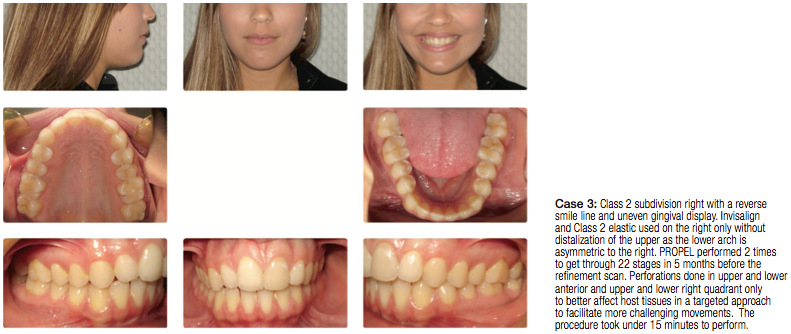
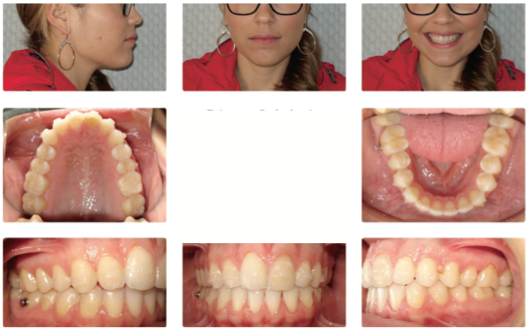
PROPEL product overview
Bi-Products of Excelleration: The Excellerator and Excellerator RT
The most recent product innovations from PROPEL are the Excellerator and the Excellerator RT. Both offer improvements over the first generation devices that were first launched in the fall of 2012.
First, the tip of each is much sharper than the first-generation device, making for not only easier penetration through the soft tissue and periosteum, but also the cortical plate of bone for more successful engagement of the threads into the bone. Second, the pitch angle of the threads is steeper. This improvement allows for fewer turns or revolutions of the device necessary to reach desired depths. This translates to less chairtime necessary to perform the procedure. Clinical experience tells us that four quadrants takes 15 minutes whereas several teeth take but only a few minutes to complete the procedure. This means little disruption to office scheduling.
There are several features that are unique to the Excellerator. The clinician need not worry about sterilization as it is disposable to be discarded after the patient’s office visit. Each device can be used for any number of perforations during that one visit. Desired depths can be dialed in at 3 mm, 5 mm, and 7mm by turning the clicking and locking head. Finally, once the desired depth is reached, the red LED light is illuminated, alerting the clinician that the desired depth has been reached.
The Excellerator is good for doctors who are beginning their journey into the fourth order of orthodontics and do not want to spend too much in initial armamentarium costs. Also, as mentioned, it is great for doctors who do not want to deal with sterilization procedures or who need the LED depth light as a guidance during the procedure.
The Excellerator RT has several hallmarks that make it stand apart. First, it has disposable tips that are inserted into an autoclavable metal driver head. While there may be a slight increase in initial start-up costs, the disposable tips will save you money in the long term. Second, the metal driver head has a thicker handle than its sibling device. Due to this larger diameter, some have reported that this feature makes it easier to grip and turn. Combining this with the sharper tip and higher pitch angle of the helixes truly makes the procedure effortless for the clinician. Unlike its sibling, the Excellerator RT does not have a depth-indicating light. Instead it has three depth-indicating lines on the retractable sheath with which to measure the depth of the micro-osteoperforations.
The Excellerator RT has been enjoyed by clinicians of varying experience. When choosing one over the other, it simply comes down to doctors’ preference and comfort for which device will best fit into their office systems. While there are two choices for the same solution, there is only one system that bridges the fourth order of orthodontics to the private practice in a simple, effective, and efficient manner. Excel at your practice with PROPEL and their Excellerator Series products.
References
- Linge L. Tissue reactions in facial sutures subsequent to external mechanical influences. Monograph #6, Craniofacial growth series. University of Michigan, Center for Human Growth and Development. 1976.
- Nicozisis JL, Nah-Cederquist HD, Tuncay OC. Relaxin affects the dentofacial sutural tissues. Clin Orthod Res. 2000;3(4):192-201.
- Davidovitch Z, Nicolay OF, Ngan PW, Shanfeld JL. Neurotransmitters, cytokines, and the control of alveolar bone remodeling in orthodontics. Dent Clin North Am. 1988;32(3):411-435.
- Davidovitch Z, Finkelson MD, Steigman S, Shanfeld JL, Montgomery PC, Korostoff E. Electric currents, bone remodeling, and orthodontic tooth movement. II. Increase in rate of tooth movement and periodontal cyclic nucleotide levels by combined force and electric current. Am J Orthod. 1980;77(1):33-47.
- Wilcko WM, Wilcko T, Bouquot JE, Ferguson DJ. Rapid orthodontics with alveolar reshaping: two case reports of decrowding. Int J Periodontics Restorative Dent. 2001;21(1):9-19.
- Kopher RA, Mao JJ. Suture growth modulated by the oscillatory component of micromechanical strain. J Bone Miner Res. 2003;18(3):521-528.
- Nishimura M, Chiba M, Ohashi T, Sato M, Shimizu Y, Igarashi K, Mitani H. Periodontal tissue activation by vibration: Intermittent stimulation by resonance vibration accelerates experimental tooth movement in rats. Am J Orthod Dentofacial Orthop. 2008;133(4):572-583.
- Teixeira CC, Khoo E, Tran J, Chartres I, Liu Y, Thant LM, Khabensky I, Gart LP, Cisneros G, Alikhani M. Cytokine expression and accelerated tooth movement. J Dent Res. 2010;89(10):1135-1141.
- Alikhani M, Raptis M, Zoldan B, Sangsuwon C, Lee YB, Alyami B, Corpodian C, Barrera LM, Alansari S, Khoo E, Teixeira C. Effect of micro-osteoperforations on the rate of tooth movement. Am J Orthod Dentofacial Orthop. 2013;144(5):639-648.
Stay Relevant With Orthodontic Practice US
Join our email list for CE courses and webinars, articles and mores


