
Dr. Thomas S. Shipley discusses increasing the bone remodeling rate for more rapid aligner progression
The use of clear aligners has gained broad acceptance as an alternative way to orthodontically move the dentition. As the orthodontic community becomes more familiar with this modality of treatment, questions arise as to best clinical practices to achieve optimal results. One area of interest is how often to change aligners. The Invisalign® System suggests the optimal time to change from one aligner to the next, with good patient compliance, is 2 weeks.
The aligner system and the amount of movement prescribed in each aligner determine how frequently the patient is required to change aligners in the sequence. Changing aligners at a faster rate than the velocity of tooth movement would be one cause of aligners not “tracking” over time. This rate of aligner change is a limiting factor in the overall case completion time.
In more difficult cases, the number of aligners prescribed may reach as many as 40 to 60 aligners, with even more in the most difficult cases. To the patient, who can quickly do the math, and to the clinician, who knows “refinement” or “auxiliary treatment” has not even been accounted for yet, the future of the orthodontic treatment becomes daunting. In these cases, or with any case, where increased velocity of tooth movement is desired, a way to change aligners at a more rapid pace becomes attractive.
The rate of tooth movement is dependent on the rate of the physiologic process of bone remodeling.1,2 If this rate of bone remodeling is increased, then the rate at which aligners should be changed increases also. Failing to change the aligners fast enough to coincide with the velocity of tooth movement would be equivalent to placing intermittent orthodontic forces on the dentition, which could actually slow the overall progress of the movement. Increasing the rate of bone remodeling is the key to being able to change aligners at a more rapid pace, therefore, decreasing overall treatment time.
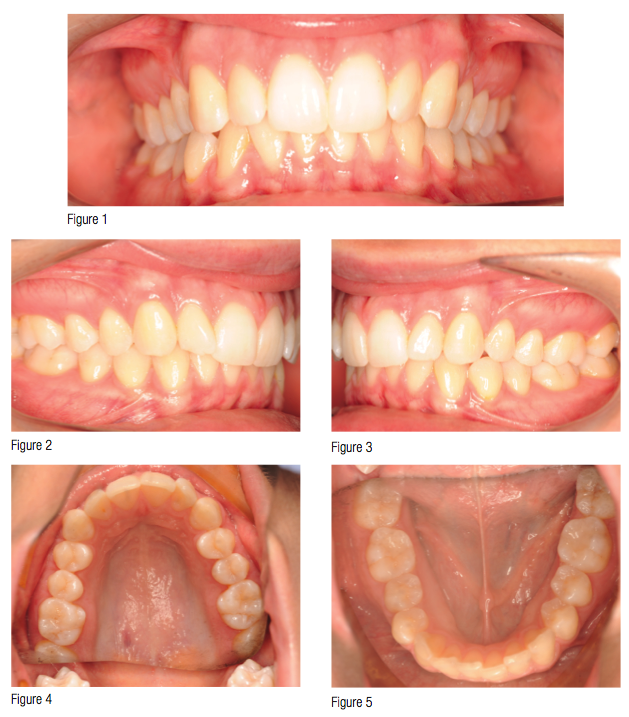
A female patient presented at age 21 with a mild Class II, Division 2 malocclusion. Moderate upper and lower dental crowding existed with a 60% deep bite and negatively inclined upper incisors. The patient’s chief concern was the rotation of the upper left lateral incisor. The CBCT showed good root parallelism and normal development of the dentition (Figures 1-7).
The treatment plan was developed to use clear aligners in conjunction with Class II elastics to resolve the dental crowding, slightly procline the upper and lower incisors, correct the deep bite, and improve the Class II dental relationship.
Once the treatment plan was finalized, the resultant prescription for aligners was 43 upper and lower aligners. The aligners consisted of 43 active maxillary aligners, and 23 active lower aligners, followed by 20 lower passive aligners (Figures 8-9). Cuts were made in the upper aligners near the maxillary canines to create hooks for Class II elastics and cutouts in the lower aligners in the buccogingival area of the lower second molars to allow for Class II button hooks to be bonded (Figure 14). No interproximal reduction was prescribed.
The patient desired to finish treatment faster than 86 weeks! The clinician was concerned that this treatment did not allow much time for refinements and detailing which may be needed. Both agreed that Propel would be an appropriate way to speed the orthodontic treatment.
Propel is a technique performed with the patented FDA Registered Class 1 5(10k)-exempt disposable medical device that creates Micro-Osteoperforations (MOPs). These MOPs stimulate a cytokine response in the patient’s alveolar bone during orthodontic treatment (Figures 10-11).3 MOPs reduce overall orthodontic treatment time by harnessing the body’s own biology to increase the rate of tooth movement and release challenging movements.4 This in-office technique can be performed chairside in minutes during a patient’s regularly scheduled office visit and can be used in conjunction with any type of fixed or removable orthodontic appliance. Micro-Osteoperforations with Propel can be used to advance the treatment of any malocclusions, including, but not limited to, crowding, space closures, molar uprighting, rotations, intrusions, and extrusions.
Aligners 1 and 2 were delivered at the initial appointment. The patient was told to wear each aligner for 2 weeks and return in 4 weeks for placement of attachments. At the 4-week return appointment, aligner 3 was delivered, attachments were placed, and Class II elastics commenced. No Propel was used for the first 6 weeks of treatment. A regular tray progression of 2 weeks per tray was used. There are several advantages to starting at this pace. The patient has ample time to adapt to wearing the trays and to learn how to be compliant. Treatment progressed at a slower pace, not to overburden the patient with learning to wear the trays, having attachments placed, beginning elastic wear, and Propel all at the same time. In addition, the clinician is given an opportunity to gauge patient compliance before beginning Propel. The enhanced cytokine response with the MOPs would be of little benefit without good patient compliance.
Six weeks into treatment, Propel was initiated. The use of local infiltration anesthesia (2% Lidocaine with 1:100,000 epinephrine) was employed. “Profound” topical anesthesia may instead be used. The patient rinsed twice with chlorhexidine gluconate and expectorated. MOPs were placed inter-radicularly using the Propel device as follows:
Three MOPs mesial and distal of the maxillary lateral incisors, and two MOPs mesial and distal of the lower incisors (Figures 12-13). She stated that there was little discomfort of the procedure other than mild pressure between the teeth in a few areas. A post-Propel CBCT was taken, which shows the location of the maxillary left MOPs (see image). The patient rinsed again with chlorhexidine gluconate after the procedure and was asked to wear the aligners at a progression of 3 days each.
With such a rapid pace of aligner progression, close monitoring by the clinician is needed to ensure patient compliance and good aligner “tracking.” If the rate of aligner progression exceeds actual tooth movement, it will be apparent due to poor aligner fit. Aligner progression may be slowed, if needed, based on how the patient presents on follow-up visits.
The patient was seen 2 weeks later and was now beginning aligner 9. As shown in the photos, the aligners were fitting the dentition perfectly (good “tracking”). This indicated that the progression at 3 days per aligner was appropriate for this patient (Figures 16-18). In addition, the soft tissue had completely healed with no signs of trauma at 2 weeks (Figures 19-20).
The patient was seen again 2 weeks later (4 weeks post-Propel). At this time, she was just beginning tray 14, and a CBCT was taken that shows the MOPs slightly smaller, but still present (Figure 21). Again, the “tracking” of the aligners was still excellent. A 4-week interval was now chosen, continuing at 3 days per aligner.
Four weeks later, the patient was wearing the 23rd aligners. The aligners were still “tracking” perfectly, and treatment was completed on the lower arch. Complete resolution of the lower dental crowding was achieved as prescribed using 23 aligners over a period of 14 weeks. No refinement or detailing was needed for the lower arch.
More aligners were delivered, and Class II elastics were continued. The patient returned every 4 weeks forward until completion of treatment of the maxillary orthodontic treatment. The aligner progression continued at 3 days per aligner. The patient continued to change the lower passive aligners at the same pace.
At 23 weeks, treatment was completed on the upper dentition after the use of 43 upper aligners. No refinement aligners were needed. Attachments were removed, and retainers with similar Class II elastic hooks and cutouts were fabricated. The bonded buccal hooks on the lower 2nd molars were left for 6 months, for the continued use of class II elastics for 12 hours per night as part of the retention protocol. Otherwise, the clear removable retainers were worn according to the clinician’s normal retention protocol.
Evaluation of the final records shows adequate inclination of the upper and lower incisors to allow for better anterior guidance, which was achieved by upper anterior labial crown torque and lower incisor proclination aided by the use of Class II elastics. In addition, the overbite was corrected to an appropriate 30%. The patient’s chief concern of the rotated upper left lateral incisor was completely corrected to her satisfaction, along with complete resolution of the remaining upper and lower dental rotations. The post-treatment CBCT, taken 6 months post-Propel, shows the MOPs almost complete healed (Figure 25).
The final results show that Propel is a good approach to increasing the rate of clear aligner progression by increasing the rate of bone remodeling. Treatment time was reduced over 70% in this case as compared to a typical 2 week interval aligner case. The overall amount of appointments were reduced from 20+ to 8. More research is needed to gain a better understanding of the exact rate of tray progression that should be used. A clinician new to this treatment modality should consider starting at a slower progression than that shown with this case, such as 7 days per aligner. Close monitoring should be employed, and adjustments may be made to the rate of progression based on the clinical results for each patient.
References
1. Henneman S, Von den Hoff JW, Maltha JC. Mechanobiology of tooth movement. Eur J Orthod. 2008;30(3):299-306.
2. Krishnan V, Davidovitch Z. On a path to unfolding the biological mechanisms of orthodontic tooth movement. J Dent Res. 2009;88(7):597-608.
3. Teixeira CC1, Khoo E, Tran J, Chartres I, Liu Y, Thant LM, Khabensky I, Gart LP, Cisneros G, Alikhani M. Cytokine expression and accelerated tooth movement. J Dent Res. 2010;89(10):1135-1141.
4. Khoo E, Tran J, Raptis M, Teixeira CC, Alikhani M, Abey M. Accelerated Orthodontic Treatment [research paper]. New York: New York University; 2011.
Gallery
{gallery}140322_Shipley{/gallery}
Stay Relevant With Orthodontic Practice US
Join our email list for CE courses and webinars, articles and mores


